Case Study
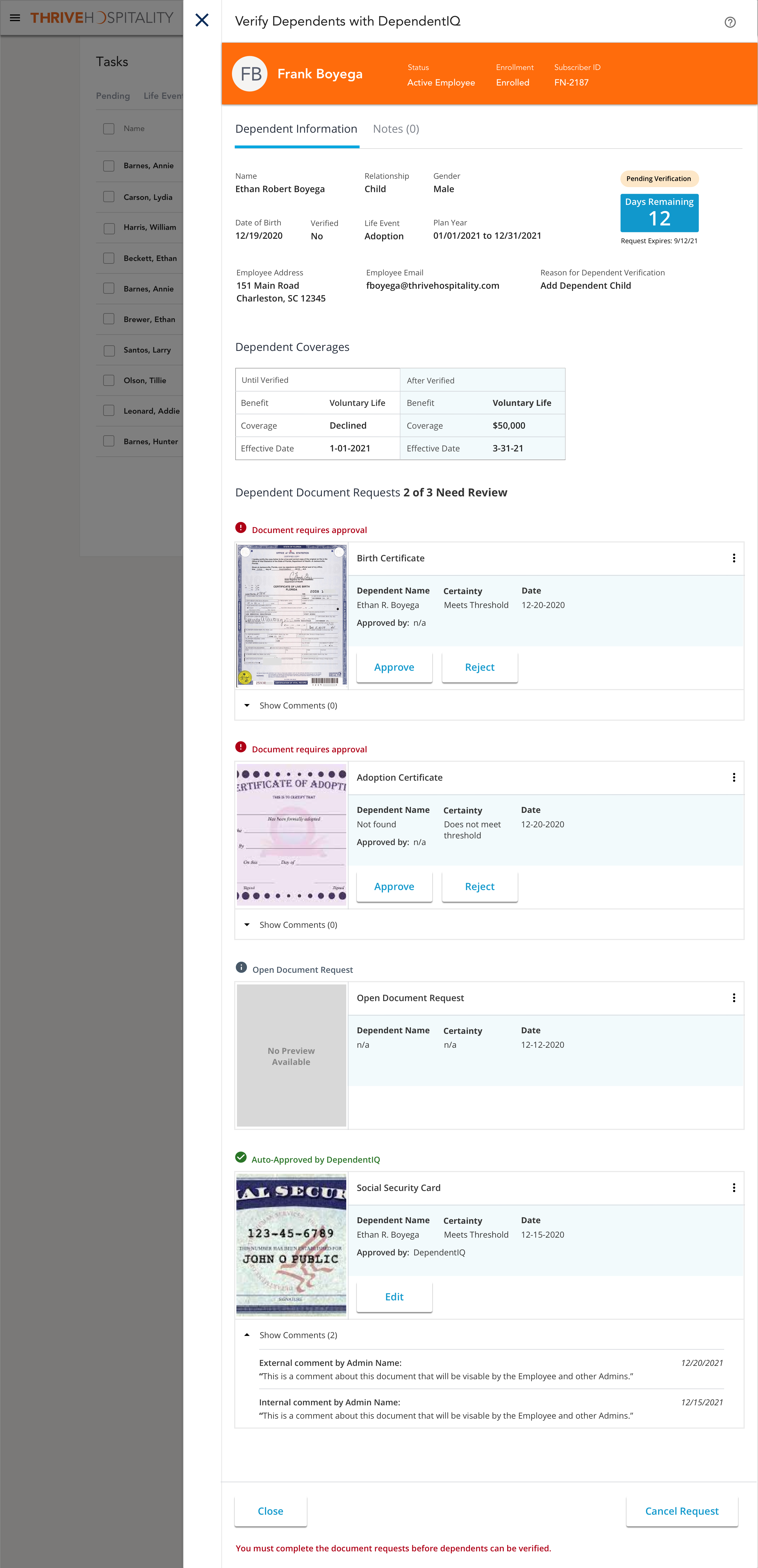
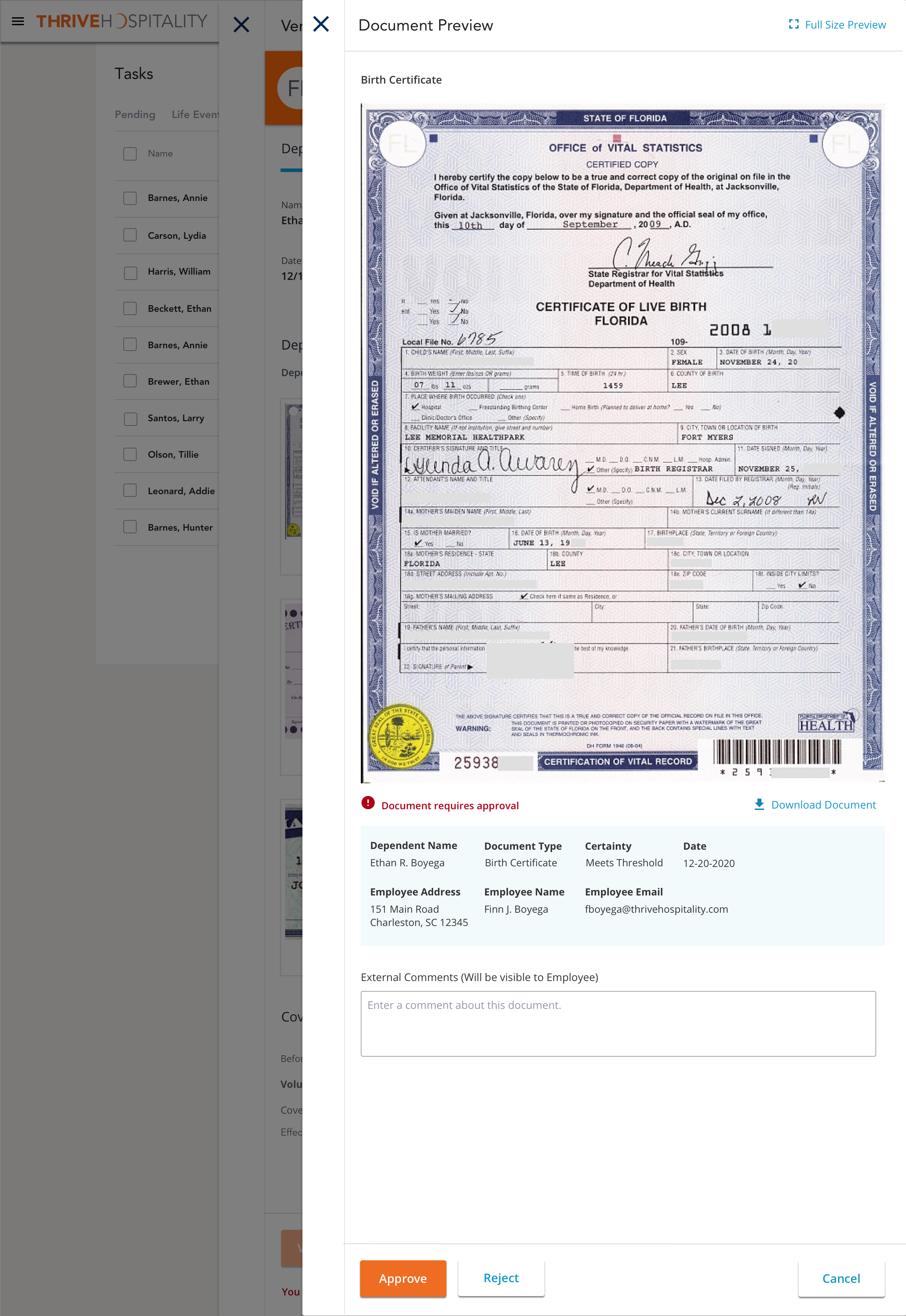
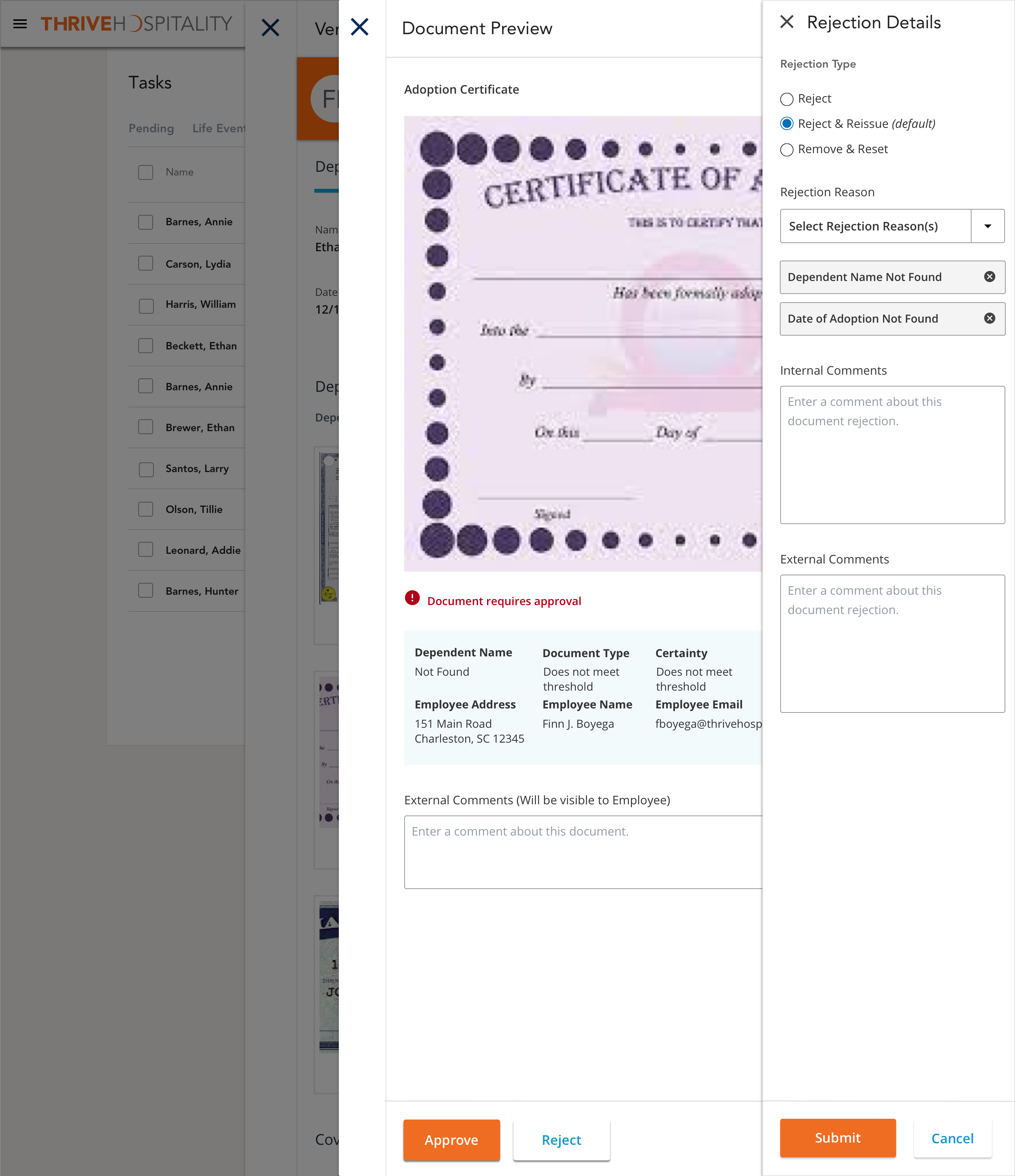
Automated Dependent Verification
Project Goal: Automating the verification process of employee's dependents for their company's health benefits through AI and machine learning capabilities.
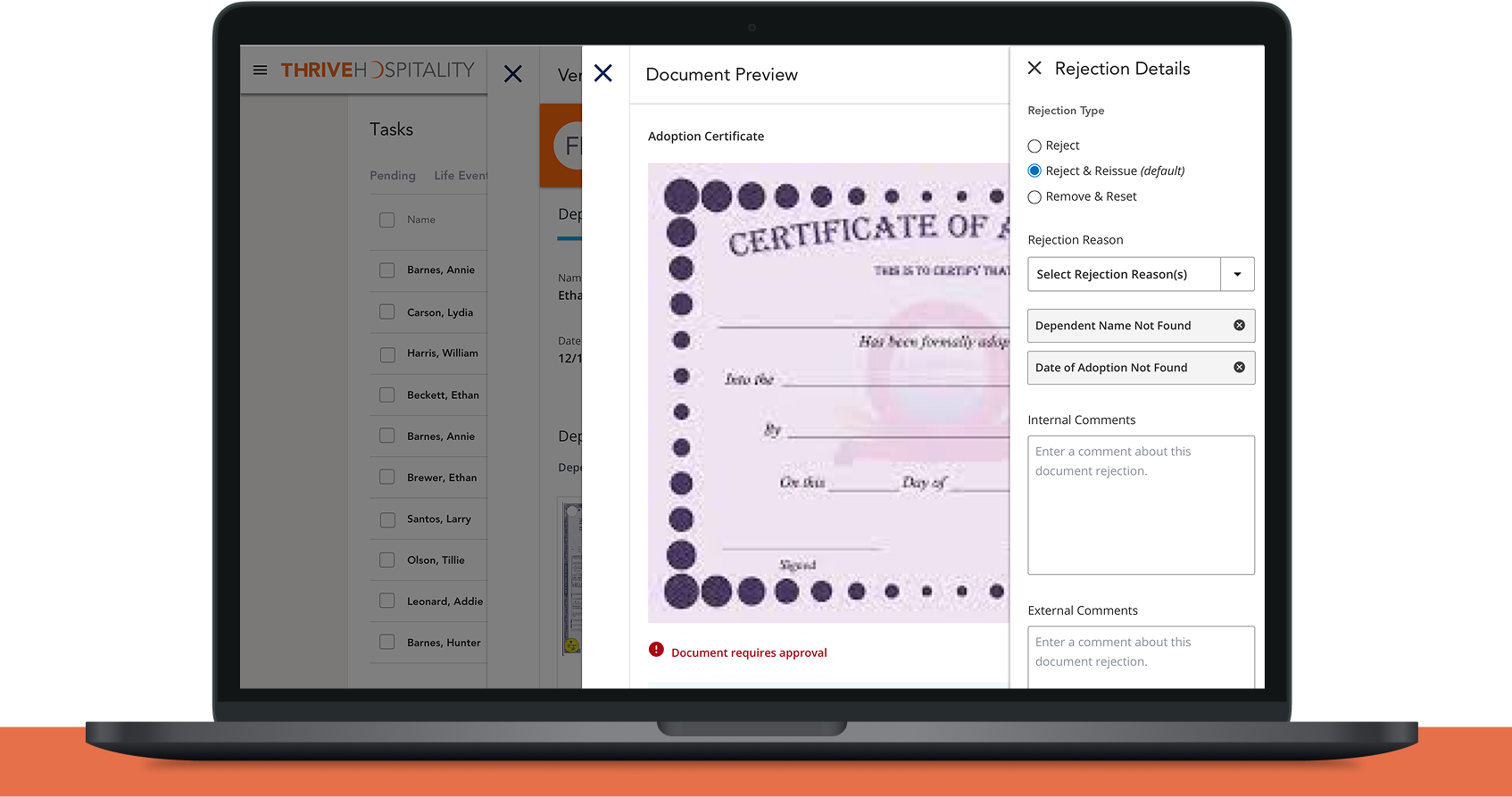
Case Study
Project Goal: Automating the verification process of employee's dependents for their company's health benefits through AI and machine learning capabilities.

UX / Visual Design / User Testing
6 Months
Research, Wireframes, Prototypes, UI/UX Design
The Problem
Dependents that get mistakenly verified for coverage when they are actually ineligible can cause thousands of dollars per year per employee. This can add up very quickly, so by using the power of our AI / ML engine we can eliminate these verification errors and save our users millions over time.
Research insights
By using the power of our AI / ML engine we can eliminate these verification errors and save our users millions of dollars over time.